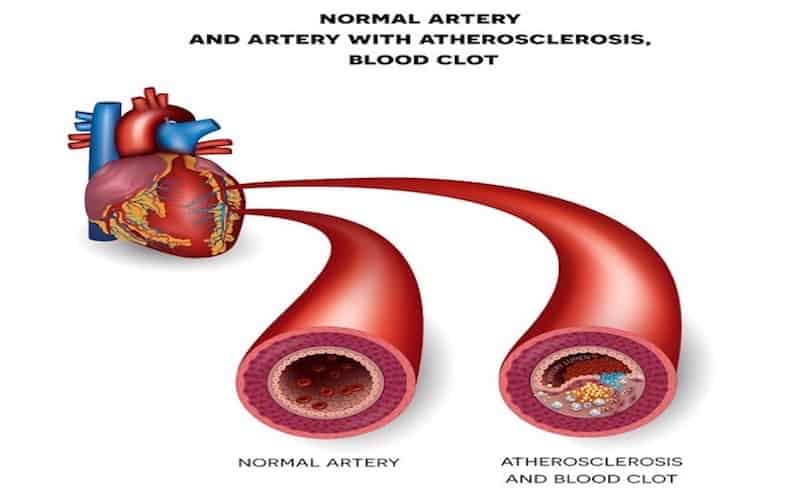
Vascular Specialist fun fact: If our blood vessels were stretched end-to-end, they would wrap around the Earth twice. This system of cosmic proportions made up of flexible tubes, large and minuscule, makes up the vascular circulatory system. Vein and Artery Health is the mission of vascular surgeons.
Any abnormal condition that impacts this system is considered to be vascular disease. You might imagine that vascular specialists focus solely on diseases that impact the vascular system, but that’s not necessarily the case.
Read on to learn more about the conditions treated by a vascular specialist, and the circumstances under which you should consult one.
What Do Vascular Specialists Do?
From varicose veins to strokes, a vascular specialist specializes in the care of a variety of vascular problems and conditions of the circulatory system, with the exception of conditions that impact the heart and brain. Vascular specialists treat blood vessels as well as the lymphatic system, which is a part of the immune system that maintains fluid balance.
A vascular surgeon is trained in every possible form of vascular intervention and surgery. However, they don’t just focus on or push surgical procedures. They ensure that patients with vascular health issues understand all their options.
Many vascular conditions can be treated with medication or changes in lifestyle, exercise, and diet. But when surgery is necessary, a vascular surgeon doesn’t just perform the surgery and then leave.
A vascular surgeon builds a relationship with each patient; after all, vascular disease can be a long-term condition. It’s important that you feel comfortable with your doctor and are certain that they have your best interest at heart.
Additionally, vascular specialists can treat chronic or non-healing wounds. As many as 6.7 million Americans suffer from non-healing wounds— these range from amputees to cancer survivors and everything in between.
Some vascular specialists are also trained in wound care, and they’re able to help speed up the healing process and generally improve the patient’s quality of life as well as prevent a recurrence of the wound.
When Should You See a Vascular Specialist?
The short answer? You should see a vascular specialist when you are diagnosed with a vascular condition or when you exhibit common symptoms of vascular disease. Typically, a primary care physician or podiatrist provides a referral to a vascular specialist. For instance, you may see your regular doctor for pain and swelling in your leg and discover that you have deep vein thrombosis.
However, if you fall into one or more high-risk categories—if you’re a smoker, diabetic, or have high blood pressure— you might consider developing a relationship with a vascular specialist as a precaution. Then, should a problem arise, you’ll have a doctor who has a full understanding of your medical history.
3 Common Types of Vascular Conditions
There are a variety of vascular conditions, but here are the three that occur most frequently.
#1: Pulmonary embolisms and blood clots
Blood is always flowing inside your body. But sometimes it doesn’t move as well as it should— perhaps after surgery, during pregnancy, or when you’re sitting for long periods of time. When that happens, you may be at risk for deep vein thrombosis, or DVT.
Your veins rely on the movement of neighboring muscles as well as your heartbeat to move blood through them. Veins have valves that prevent blood from flowing backwards and pooling in your arms and legs. When your blood flow slows down, sticky substances called clotting factors form, making blood cells clump together. DVT occurs when those sticky cells form a blood clot.
A blood clot can build up in a vein (usually in the leg) and break apart. If a broken part of the clot enters your bloodstream, it travels through veins in your belly and into your heart and then into your lungs. The blood clot can get stuck and block the blood vessels. This serious condition, called pulmonary embolism, can permanently damage your lungs and even cause death.
Symptoms include:
- shortness of breath
- sharp pain in chest
- dizziness, lightheaded
- coughing up blood
#2: Pelvic Congestion Syndrome (PCS)
An estimated 15% of women between the ages of 20 to 50 experience chronic pelvic pain related to pelvic varicose veins. However, thousands of women suffer from this condition without understanding exactly where the pain is coming from!
PCS creates extreme discomfort when women sit or stand, thanks to the dilation of ovarian and/or pelvic veins or blockage of the upper iliac vein, which is nearest to the pelvic area. When women experiencing PCS lie down, the discomfort disappears— the vein is decompressed and the pressure is alleviated. This makes it hard to diagnose.
After a thorough gynaecological examination that rules out all other potential pelvic issues, patients are referred to a vascular specialist, who can diagnose PCS through minimally invasive methods, including MRI, ultrasound, pelvic venography, or intravascular ultrasound.
#3: Stroke
Stroke strikes about 700,000 Americans each year, but the vast majority of people survive. Close to 5 million stroke survivors are managing their health today, thanks to the help of vascular specialists.
Disruptions of blood circulation to the brain may result in a stroke. There are three major kinds of stroke: ischemic, hemorrhagic, and TIAs (mini-strokes) – each with different warning signs and symptoms.
Sudden warning signs of stroke include:
- numbness or weakness
- confusion
- dizziness
- severe headache
This is not an exhaustive list of vascular conditions, and in no way should be used as a substitute for medical advice or treatment. If you have experienced any of the symptoms mentioned here, consult with your physician immediately.
If you’re experiencing any vascular condition, from varicose veins to peripheral arterial disease (PAD), or you’re struggling with a chronic or non-healing wound, the physicians at Maryland Vascular Specialists can help. Just click here to request a free consultation with one of our experts today.