How to Prevent 6 Diabetes-Related Vascular Challenges
It is known that diabetics face a lot of challenges, and managing their health is one of the top challenges. While a diagnosis of diabetes is a life-altering event, the good news is that diabetes can be successfully managed if you consistently make the lifestyle and health changes that are recommended by your doctor. The daily health checklist for every diabetic should include: monitoring your blood sugar, checking your feet for ulcers and infection, and being aware of any changes in your eyesight. In addition, since diabetics have the greatest risk for developing vascular disease of any form, it is important for them (and their caregivers) to know how to prevent the six diabetes-related vascular challenges that we have outlined below. The ultimate goal is to have people with diabetes manage this condition and stay in good health.
Diabetes & Blood Circulation
Newly diagnosed diabetics and their caregivers need to understand the magnitude of what diabetes can do to the body. High blood sugar (hyperglycemia) is one of the most dangerous factors of diabetes. Many people do not realize that elevated blood sugar levels affect the blood vessels throughout the body. When your blood vessels cannot send oxygen-rich blood to every part of the body, the consequences can be severe.

Prevention Tips for 6 Diabetes-Related Vascular Challenges
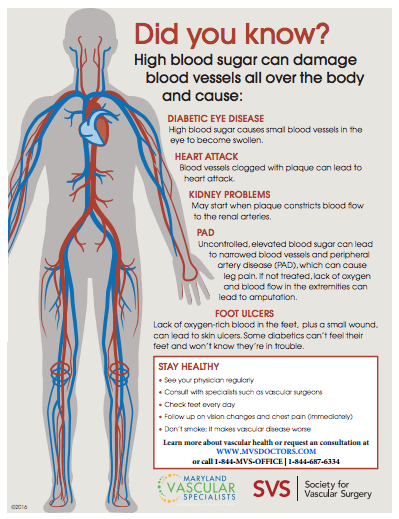
1. Diabetic Eye Disease – This disease affects diabetics only and occurs when the retinal blood vessels swell and block oxygen to the eye. Diabetic eye disease can cause blindness if it is not treated.
Prevention Tip: It is important to consult your eye doctor if you notice any changes in your vision. It is also recommended that you schedule a dilated eye exam once a year with your medical practitioner.
2. Peripheral arterial disease< (also known as PAD) – This disease is fairly common in people over 55 years old, and even more likely among diabetics, as diabetes increases plaque buildup in the arteries. PAD is a potentially life-threatening condition if left untreated. It is a result of plaque that builds up in the walls of your arteries, which subsequently slows down the blood flow to your legs and feet. To learn more about PAD risks, prevention, symptoms, and treatment options, click here to download our FREE e-Book.
Prevention Tip: Taking a walk on a daily basis is often the first step to take, as long as you have no other health issues or an ulcer on your foot that would prevent from doing so. Daily walks can be both preventive and a first level treatment for peripheral arterial disease. Walking increases blood flow to the legs and feet and can aid in decreasing leg pain. Before starting any exercise plan, be sure to discuss it with your doctor. Patients who have PAD symptoms should also have regular checkups with a vascular surgeon.
3. Foot ulcers and peripheral neuropathy – Diabetic foot ulcers are very serious and should not to be taken lightly. While diabetic foot ulcers can form as a result of PAD or PAD complications, they are also caused by peripheral neuropathy ( a lack of feeling in the legs and feet) which is also caused by diabetes. When there is a lack of feeling in their feet, diabetics may not realize that there is an open cut or ulcer on the foot. If this is not treated, it can lead to infection or even amputation.
Prevention Tip: It is important to do foot checks daily to ensure there are no cuts or open wounds to your feet, and to wear proper diabetic footwear. If you discover an open cut or wound on your foot, it is critical to schedule an appointment with your podiatrist and your vascular specialist to be evaluated and treated immediately.
4. Smoking – Smoking is obviously a bad habit, and there are no benefits to doing it. Smoking causes damage to every part of the body including your blood vessels, and the risk for health complications are substantially greater for diabetics who smoke. Smoking constricts blood vessels, causes inflammation, and causes plaque to build up on artery walls. This can lead to various vascular conditions such as peripheral arterial disease (PAD) and deep vein thrombosis (DVT).
Prevention Tip: If you are a smoker, seek help to stop smoking immediately. It can be hard to quit smoking, but for diabetics, it is a must! Here are some resources to help you stop smoking: SmokeFree, Be Tobacco Free, SmokeFree Women, and the American Lung Association Quit Line.
5. Heart attack – Diabetes affects every artery in the body, including the arteries that supply the heart with blood; therefore, diabetics have an in increased risk of heart attacks. People who have both diabetes and heart disease may not have typical symptoms of heart disease such as activity-induced chest pain (angina).
Prevention Tip: It is critical that you monitor your weight, blood sugar, and cholesterol levels. If you experience any chest pain, shortness of breath, or inability to do exercise, contact your doctor for an appointment as soon as possible.
6. Renovascular conditions – Kidneys have blood vessels, so they are susceptible to the effects of diabetes just like the rest of your body. The renal arteries originate in your heart and are responsible for carrying blood rich in oxygen and nutrients to your kidneys. When the renal arteries become blocked, a condition called renal artery stenosis, your kidneys do not receive enough blood or oxygen. Diabetes can lead to the need for dialysis, a kidney transplant or kidney failure. Often, there are no symptoms of blocked kidney arteries until it becomes an advanced stage of kidney failure or is non-reversible.
Prevention Tip: Making sure your blood sugar, as well as blood pressure, are under control will reduce the risk of diabetes-related kidney failure. It is important to see your doctor for regular checkups and blood tests. As a diabetic, having your blood tested regularly can be beneficial in helping to detect kidney failure in its early stages. If a physician discovers an issue with your kidney in the early stages, it may be treatable with medications that could prevent kidney failure and the need for dialysis.
DO YOU HAVE DIABETES AND LEG PAIN, LEG CRAMPS, OR FOOT WOUNDS? DON’T DELAY – SCHEDULE AN EXPERT CONSULTATION
If you feel fatigue, leg pain, or cramping in your leg that is brought on by walking but relieved when you rest; experience leg pain while resting; or have wounds on your foot that are slow to heal, do not ignore them. Be sure to contact a vascular specialist (or your primary care physician for a referral) as soon as possible.
Click here to schedule an expert consultation at Maryland Vascular Specialists– we have several convenient locations to serve you in Maryland and Pennsylvania.

